Podcast Ep 12: Drownings, Geriatrics, Bowel Obstruction, & More

The best preparation for tomorrow is doing your best today. -H. Jackson Brown Jr.
Welcome back to Episode 12! This week we once again continued our theme-based review. We focused on a few high-yield bites and envenomation. This material is easy to gloss over since we do not come across it too often clinically. Not only will this prepare you at the bedside, but it will also help you pick up a few easy points on the In-Training Exam, which, by the way, is right around the corner.

- Envenomation by a Portuguese Man O’ War is treated by immediate removal of the nematocyst followed by a salt-water wash.
- Black widow spiders have a red hourglass on their abdomen.
- Bites from a black widow spider produce a local papule with a halo. Severe symptoms include muscle fasciculations and a peritonitic abdomen.
- Brown recluse spider bites cause a papule that blisters and then necroses. Severe symptoms include renal failure, pulmonary edema, and shock.
- A pit viper snake envenomation causes local swelling and oozing from the wound. Severe envenomation can cause a DIC-like coagulopathy with hemorrhagic bullae.
Now onto this week’s podcast!
Question 1
A 4-year-old boy is brought to the Emergency Department after a drowning. Bystanders noted the child was underwater for less than a minute. After quickly being pulled up from the bottom of the pool, he coughed and vomited once. He arrived at the ED awake and alert with a GCS 15. On examination, he is afebrile with heart rate 105 beats/minute, respiratory rate 20 breaths/minute, and oxygen saturation 96 % on room air. His lungs are clear to auscultation. What is the next step in management?
A. Admit to telemetry unit for 24-hour observation
B. Discharge home
C. Observe for 4–6 hours and discharge home if there is no change in his clinical status
D. Positive pressure ventilation
Question 2
Which of the following is true regarding older patients with abdominal pain in comparison to younger patients?
A. More likely to need an emergent surgical procedure
B. More likely to present with an elevated white blood cell count
C. More likely to present with fever
D. More likely to present with peritoneal signs
Question 3
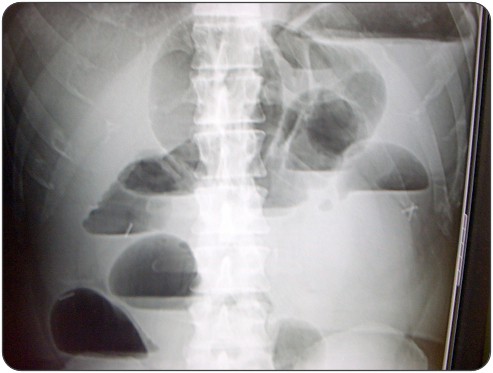
Which of the following conditions, other than postoperative adhesions, is most likely responsible for causing the diagnosis seen in the image above?
A. Adenocarcinoma
B. Incarcerated hernia
C. Intussusception
D. Volvulus
Question 4
How do you calculate mean arterial pressure (MAP)?
A. MAP = [DBP + (2 x SBP)]/3
B. MAP = DBP + 1/3(SBP-DBP)
C. MAP = DBP + 2/3(SBP-DBP)
D. MAP = SBP + 1/3(SBP-DBP)
Question 5
A 23-year-old man presents with chest pain after a motor vehicle collision. The patient’s chest struck the steering wheel. He has no other complaints or injuries. Chest X-ray is unremarkable. ECG shows sinus tachycardia with anterior ST depressions. A troponin is sent and is positive at 3.50 mg/dl. What management is indicated?
A. Activate the cardiac catheterization laboratory
B. Discharge home with cardiology follow up
C. Echocardiogram
D. Pericardiocentesis
Question 6
Which of the following mechanisms of hypoxemia is associated with the failure of arterial oxygen levels to increase in response to supplemental oxygen?
A. Diffusion impairment
B. Hypoventilation
C. Right-to-left shunt
D. Ventilation-perfusion mismatch
Question 7
A 19-year-old man presents with an ulcer on his penis. He denies pain, tenderness, and itching of the ulcer. He also denies penile discharge and dysuria. Genital examination reveals a clean-based, sharply defined, circular ulcer on the shaft of his penis. There are no other rashes or lymphadenopathy. Which of the following organisms is the most likely cause of his symptoms?
A. Borrelia burgdorferi
B. Haemophilus ducreyi
C. Plasmodium falciparum
D. Treponema pallidum

- When caring for a drowning victim with normal vitals and abnormal exam, a 4 to 6 hour observation period is sufficient before discharge. Any oxygen requirement or pulmonary finding on exam requires admission.
- Elderly patients with abdominal pain are more likely than younger patients to require an emergent surgical procedure.
- The two most common causes of SBOs are adhesions followed by cancer.
- Large bowel obstructions are caused most commonly by cancer followed by volvulus.
- Mean arterial pressure is defined as Cardiac Output x Systemic Vascular Resistance + Central Venous Pressure. It is often approximated by two-thirds of the diastolic blood pressure plus one-third of the systolic pressure.
- Myocardial contusions are a sequela of blunt chest trauma. The most common EKG finding is sinus tachycardia. These patients require an echocardiogram. The most common course is spontaneous resorption of resolution of the symptoms. The most serious complication is delayed rupture.
- The hypoxemia of right-to-left shunt would not improve substantially with supplemental oxygen and the A-a gradient would be increased.
- Diffusion impairment occurs as a result of interstitial disease which improves with supplemental O2 and has a large A-a gradient
- Hypoventilation occurs during drug overdoses, CNS lesions, and neuromuscular junction disorders. Hypoxemia in this setting improves with supplemental oxygen, and the A-a gradient is usually normal.
- In V-Q mismatches, hypoxemia improves with supplemental oxygen, and there is an increased A-a gradient.
- There are three painless penile lesions to remember: The small, shallow ulcer of LGV caused by Chlamydia. The beefy red ulcer and painless papule of Granuloma Inguinale caused by Klebsiella. Lastly the painless chancre of Syphilis caused by Treponema pallidum.
- The two painful penile lesions are the multiple painful papules that ulcerate of Chancroid caused by H. ducreyi and the shallow tender painful lesions of Genital Herpes caused by HSV.
Hope you enjoyed this week’s episode. Send us feedback and comments to Roshcast@roshreview.com. Do not forget to check out the high-yield questions and explanations in the Rosh Review Emergency Medicine Qbank.
Until next time,
Jeff and Nachi
P.S. If you missed last week’s episode including mushroom toxicity, listen here.
Get Free Access and Join Thousands of Happy Learners
You must be logged in to post a comment.





Comments (0)