Rapid Review: Transient Tachypnea of the Newborn

Reviewed January 2024
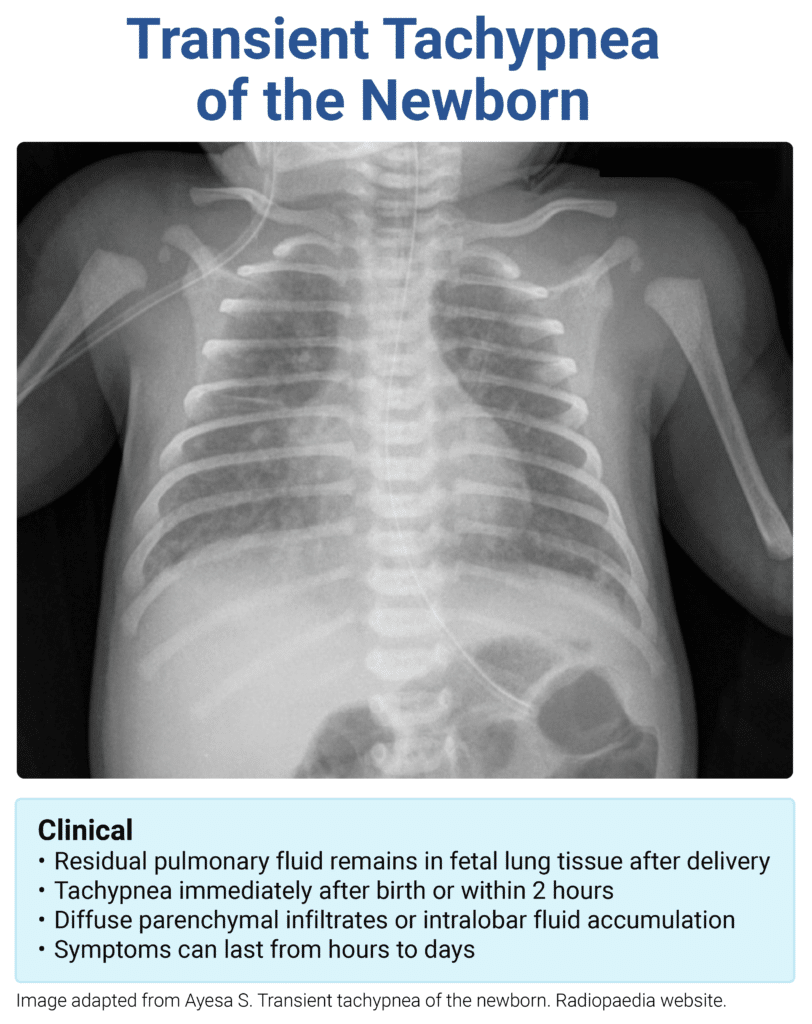
Transient Tachypnea of the Newborn
- Most common cause of neonatal respiratory distress
- RF: C/S, IDM, maternal obesity, precipitous delivery
- Cause: delayed clearance of fetal lung fluid
- PE: early onset tachypnea, nasal flaring, retractions, and hypoxia
- CXR: parenchymal infiltrates and fluid in the pulmonary fissures
- Tx: supportive, self-resolving within 72 hours
Sample question:
A 3,500 g male infant is born via scheduled cesarean delivery at 41 weeks of gestation to a G2P2 mother with a past medical history of asthma. He develops mild respiratory distress shortly after birth. Vital signs include T 37.2°C, P 140 bpm, R 75/minute, and SpO2 95% on room air. Physical examination reveals nasal flaring, mild intercostal retractions, and cyanosis. Auscultation of the lungs is normal and heart sounds are normal. Chest radiograph reveals hyperinflation, a flattened diaphragm, and prominent vascular markings in a sunburst pattern originating from the hilum. Supplemental oxygen is provided and symptoms resolve within four hours. Which of the following is the most likely diagnosis?
Get Free Access and Join Thousands of Happy Learners
You must be logged in to post a comment.





Comments (0)